What Should You Know About MRI Insurance Coverage?
Getting an MRI ordered by your doctor feels like the straightforward part. The harder conversation often comes shortly afterward, when you start figuring out what your insurance will actually pay for and what you will owe out of pocket. MRI coverage is one of the most frequently misunderstood areas of health insurance, and patients who go in without a clear picture often end up surprised by bills they were not expecting.
The complexity comes from several directions at once. Not all MRI scans are treated equally by insurance. The facility where you have the scan matters. The specific type of scan ordered matters. Whether the scan is considered medically necessary according to your insurer's criteria matters. And for patients seeking more advanced imaging, such as positional or upright MRI, there are additional coverage questions that are worth understanding before scheduling.
Quick Answer: MRI insurance coverage depends on your specific plan, the type of scan ordered, the facility used, and whether your insurer considers the scan medically necessary. Standard MRI scans at in-network hospital-based facilities are typically covered, often after meeting a deductible. Advanced positional scans and upright MRI are more frequently excluded or require prior authorization, leading many patients to explore self-pay alternatives that can be more affordable than using insurance at an out-of-network facility.
Why MRI Coverage Is Not Automatic
A doctor's order for an MRI is a clinical recommendation, not an automatic insurance approval. Most plans require the scan to meet their definition of medical necessity before they will pay for it. This is assessed against criteria set by the insurer, which may or may not align with your physician's clinical reasoning. The disconnect between what a doctor recommends and what an insurer approves is one of the most frustrating realities of navigating MRI coverage.
Prior authorization is a common barrier. Many plans require a separate review process where the clinical justification for the scan is assessed before it is approved. This adds time and administrative work, and it can result in a denial even when the scan is clearly clinically warranted. Patients who have a scan without confirming authorization first sometimes receive the full bill retroactively.
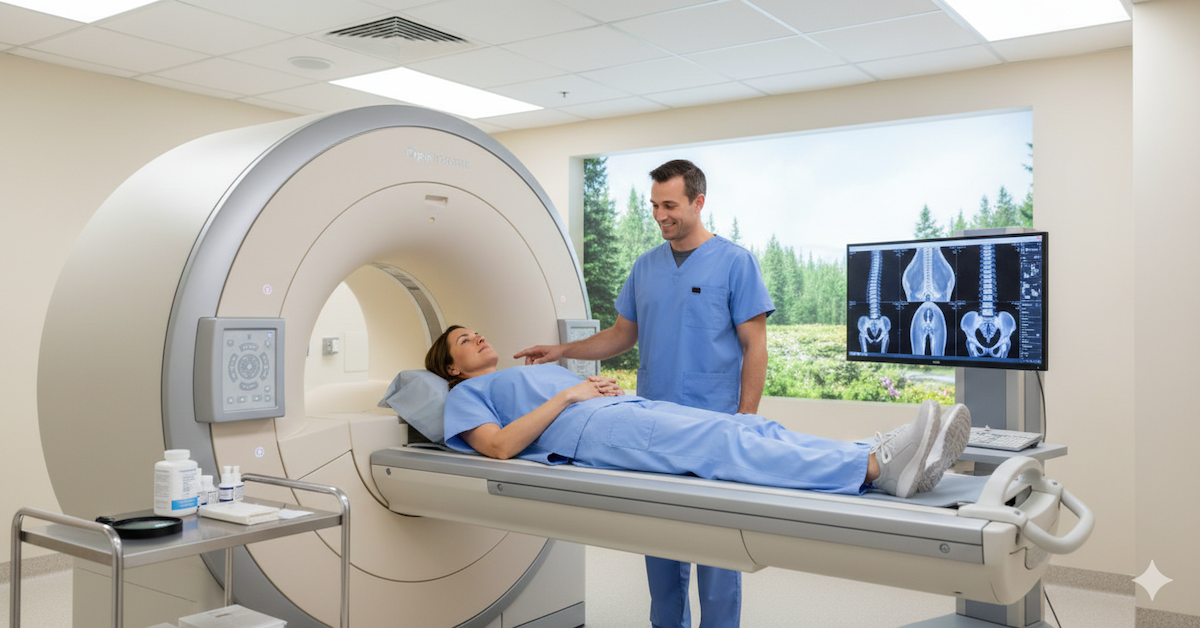
Understanding what actually happens during an MRI and how the type of scan affects both the clinical value and the insurance classification helps patients have better-informed conversations with both their doctors and their insurers.
How Deductibles, Copays, and Coinsurance Affect What You Pay
Even when a scan is covered, what you actually pay depends on where you are in your deductible cycle, the copay or coinsurance rate for imaging, and whether the facility is in-network. A scan that costs the insurer several hundred dollars can cost the patient far more if the deductible has not been met, which is common early in the plan year.
In-network versus out-of-network status is one of the most significant cost variables. An MRI at an out-of-network facility may be covered at a much lower rate or not at all, leaving the patient responsible for a large portion of the bill. Some patients discover that their physician referred them to an out-of-network imaging center without making that clear, which is a situation worth checking before the appointment rather than after.
Hospital-based imaging departments typically have higher facility fees than standalone outpatient imaging centers, even when both are in-network. The same scan performed at a hospital can cost significantly more than the identical scan at a freestanding center. Patients who call ahead to compare costs often find meaningful savings by choosing an outpatient facility.
When Advanced Positional MRI Scans Fall Outside Coverage
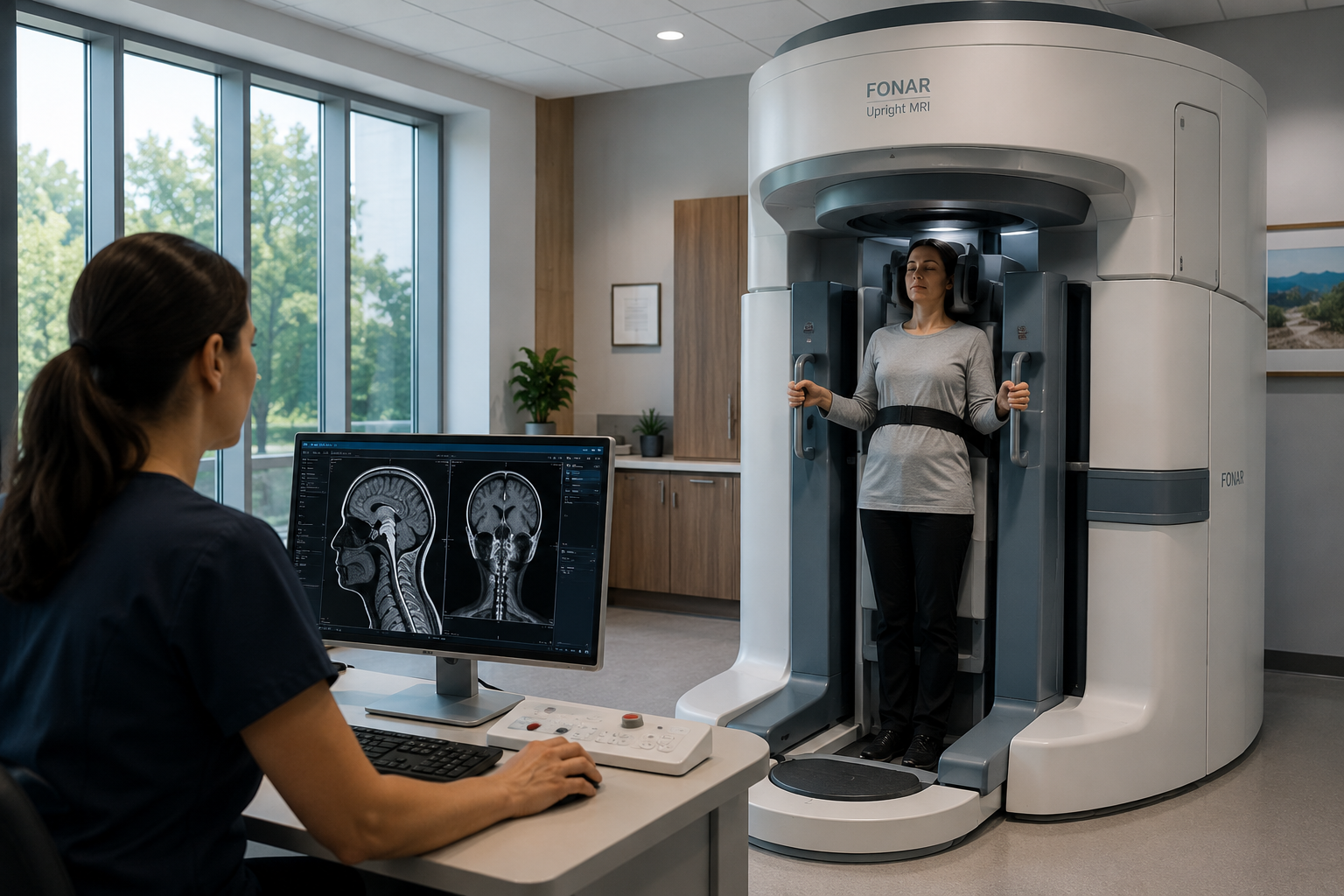
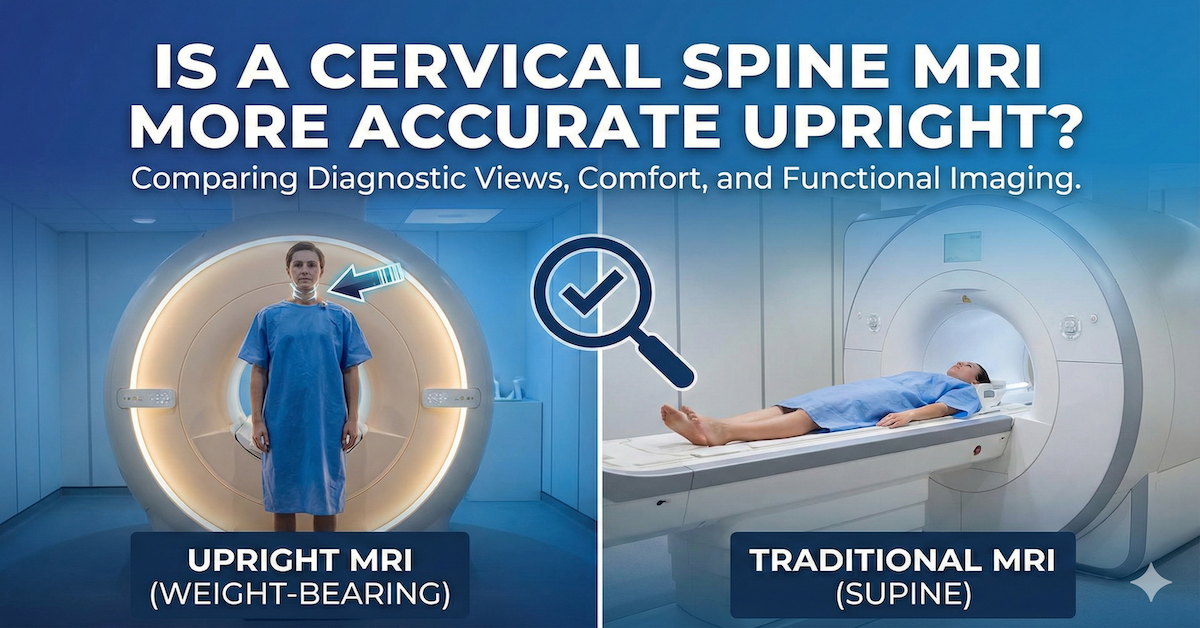
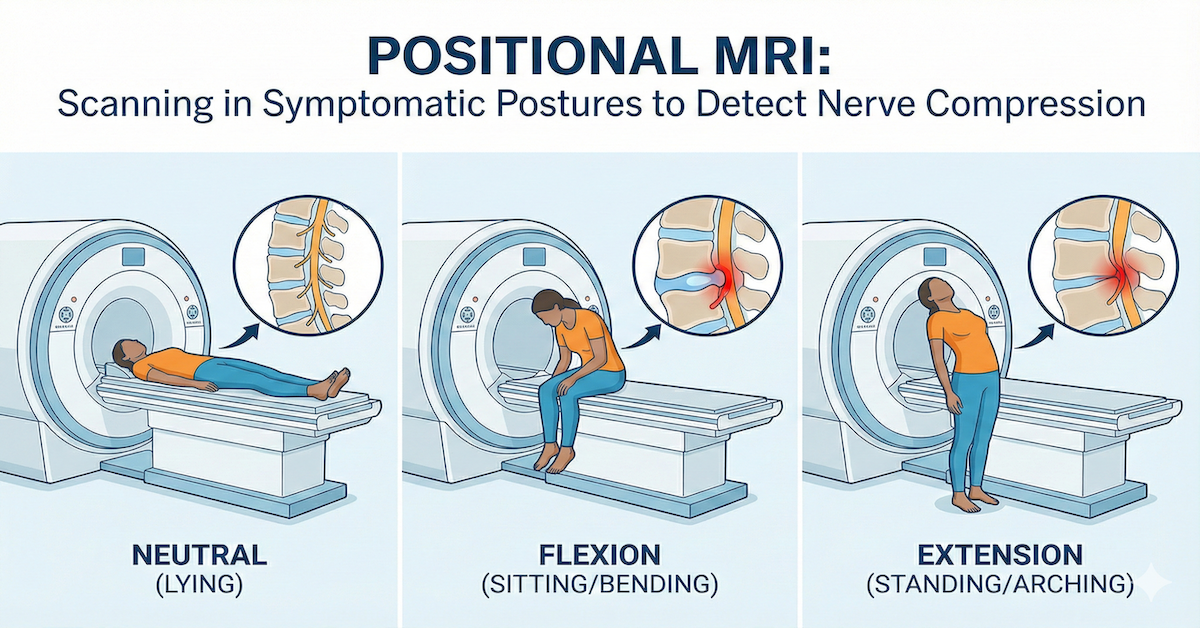
One area where insurance coverage becomes particularly complicated is advanced positional imaging. Many standard MRI plans are built around the assumption of a conventional, lying-down scan. Advanced positional scans lose coverage in many plans because insurers classify them as investigational or not medically necessary under their standard criteria, regardless of what the referring physician recommends.
The difference between upright and traditional MRI is clinically meaningful for many conditions, but insurance coverage has not always kept pace with the diagnostic evidence. Patients who need positional imaging for conditions like spinal instability, Chiari malformation, or cranio-cervical instability often find that their insurer's coverage criteria have not yet incorporated the clinical literature that supports these scans.
The result is that a scan that could provide genuinely important diagnostic information is sometimes excluded from coverage not because it lacks clinical value but because the insurer's coverage policies have not been updated to reflect current evidence. This creates a situation where the financially conscious choice under the insurance system is not necessarily the diagnostically optimal one.
Understanding Prior Authorization
Prior authorization, or pre-authorization, is the process by which an insurer reviews a requested scan before approving payment. It is required for many MRI scans under most major insurance plans and failing to obtain it in advance typically results in a significantly reduced benefit or no coverage at all.
The prior authorization process involves the treating physician's office submitting documentation supporting the medical necessity of the scan. This documentation is reviewed against the insurer's criteria, which vary by plan. Approval is not guaranteed, and denials are common for scans that fall outside the insurer's standard criteria, including some types of positional imaging.
Patients who receive a denial can appeal, and appeals are sometimes successful, particularly when the referring physician provides detailed documentation of why the specific scan is clinically necessary for this individual patient. However, the appeals process takes time and adds burden to an already difficult situation for many patients.
Self-Pay MRI: When It Makes More Sense Than Using Insurance
For patients whose insurance does not cover the scan they need, or whose out-of-pocket cost through insurance would be high, self-pay MRI options are often more affordable than people expect and can be arranged quickly without the administrative delays of authorization and appeals.
Many patients are surprised to find that out-of-pocket access to specialized scans at a facility like Upright MRI of Deerfield costs less than what they would owe through their insurance after applying their deductible and coinsurance, particularly early in the plan year when deductibles have not yet been met.
The self-pay pathway also typically means faster scheduling, no authorization delays, and the ability to choose the specific type of scan that the patient and physician believe is most clinically valuable rather than defaulting to whatever the insurer will cover. For patients with complex or unusual presentations where standard imaging has not been sufficient, this flexibility can be genuinely important.
A concierge MRI service takes this a step further by providing a coordinated, personalized experience that removes the typical administrative friction from start to finish, including detailed consultations to help patients understand what scan is most appropriate for their specific situation.
Questions to Ask Before Scheduling
Patients who ask a few specific questions before scheduling an MRI typically avoid the most common coverage surprises. The most useful questions to ask your insurer are: Is this facility in-network? Is prior authorization required for this scan? What is my current deductible balance, and will this scan apply to it? What is my coinsurance rate for outpatient imaging?
The common questions about the process at Upright MRI of Deerfield also address what patients can expect when navigating the practical steps of scheduling, what to bring, and how results are communicated.
If there is any chance you will need a positional or advanced scan, asking your insurer specifically about coverage for upright or weight-bearing MRI before scheduling is worthwhile. Many patients discover the coverage situation only after the scan has been performed, which leaves fewer options for managing the cost.
Frequently Asked Questions
Does Medicare cover upright MRI scans?
Medicare covers MRI when it is deemed medically necessary and ordered by a qualified physician. Coverage for upright or positional MRI is less consistent and depends on the specific coding and clinical justification provided. Patients receiving Medicare should confirm coverage in advance with their specific plan administrator.
Can I use my HSA or FSA to pay for an MRI?
Yes. Health savings accounts and flexible spending accounts can generally be used to pay for MRI scans that are ordered for a medical reason, including self-pay situations where insurance does not cover the scan. This is a useful option for patients who are paying out of pocket.
What does it mean when an MRI is denied for lack of medical necessity?
A medical necessity denial means the insurer reviewed the documentation submitted and determined the scan does not meet their criteria for coverage. This is not a clinical judgment on the physician's recommendation. Patients can appeal with additional documentation from their treating physician.
How much does a self-pay MRI typically cost?
Self-pay MRI costs vary significantly by location, facility type, and scan type. Standalone outpatient imaging centers like Upright MRI of Deerfield typically offer transparent self-pay pricing that is considerably lower than hospital-based imaging. Contacting the facility directly for pricing before scheduling is the most reliable approach.
Will my doctor need to reorder the scan if my insurance denies it and I decide to self-pay?
Not necessarily. The original order from your physician is typically sufficient for a self-pay scan at most facilities. Confirming this with both the facility and your physician's office before scheduling is sensible but in most cases the original order remains valid.
The Bottom Line
MRI insurance coverage involves more variables than most patients anticipate, and the gap between what is clinically recommended and what an insurer will pay for is real and common. Understanding your specific plan, getting authorization in advance, and knowing when self-pay makes more financial and practical sense gives patients the best chance of getting the scan they need without an unwelcome financial surprise.
Upright MRI of Deerfield offers transparent self-pay pricing, flexible scheduling, and experienced staff who can help navigate the practical questions around your scan. If you are weighing your options, reaching out for a consultation is a straightforward way to get the information you need.
SHARE THIS POST:
Leave a Comment:

The World's Most Patient-Friendly MRI. A comfortable, stress-free, and completely reliable MRI scan. We offer patients an open, upright, standup MRI experience that helps those who are claustrophobic and stress being in a confined area. Upright MRI of Deerfield is recognized as the world leader in open MRI innovation,
Our Recent Post

READ PATIENT TESTIMONIALS
Upright MRI of Deerfield.
Susan D.,
Highland Park, 39
I am going to tell everyone about your office! This was a great experience after I panicked in other MRI machines and had to leave. Thank you so much.

Judith B.,
Milwaukee, 61
I suffer from vertigo and other MRIs do not work. This was wonderful…absolutely NO discomfort at all. The MRI was so fast…I wanted to stay and watch the movie! Mumtaz was great. His humor really put me at ease. I’ve already recommended Upright MRI to friends.

Delores P.,
Glencoe, 55
Everything is so nice and professional with your place. I have been there a couple of times. My husband and I would not go anywhere else.